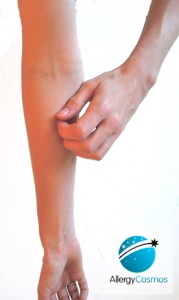
Allergic Eczema
Eczema is a dry skin condition and is closely related to dermatitis. It is most common in children however it can recur in adulthood. Eczema is not contagious but can cause swelling, redness, and itchiness to the skin and is usually found in the folds of skin in areas such as the eyes, back of the knees & neck. Allergic eczema is often triggered by common allergens like dust mite, pollen & mould.
Frequently Asked Questions
What is eczema?
What are the symptoms of eczema?
What is the prognosis of eczema?
Is there a genetic factor in eczema?
What causes atopic eczema?
What allergens produce eczema?
How is eczema diagnosed?
How can I avoid eczema 'flare up'?
What is the best long-term management?
Related Products
-
Allersearch Oatmeal Cream - Intense Relief
Regular price £16.49Regular priceUnit price per -
Allergy & Asthma Free Home Package
Regular price £65.95Regular priceUnit price per -
IQAir HealthPro 150 Air Purifier
Regular price £929.00Regular priceUnit price per -
Allersearch Allergen Wash
Regular price £22.95Regular priceUnit price per